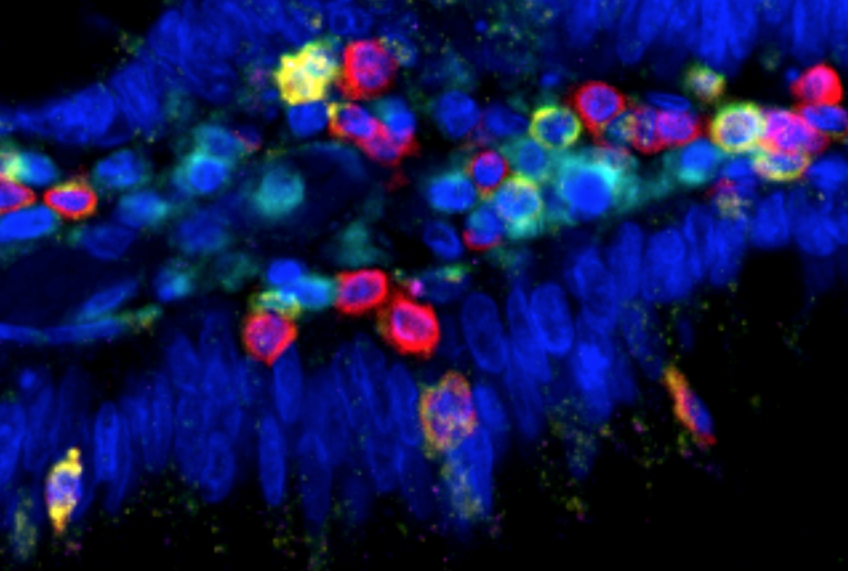
Immune evasion before tumor invasion in early lung squamous carcinogenesis
Céline Mascaux 1,2,3†,4†,5†*‡, Mihaela Angelova 6*, Angela Vasaturo 6, Jennifer Beane 5, Kahkeshan Hijazi 5, Geraldine Anthoine 4, Bénédicte Buttard 6, Françoise Rothe 7, Karen Willard-Gallo 8, Annick Haller 9†,10, Vincent Ninane 11, Arsène Burny 12, Jean-Paul Sculier4, Avi Spira 5, Jérôme Galon 6‡
1 Department of Pneumology, Nouvel Hôpital Civil, University Hospital,Strasbourg, France
2 Unité INSERM U1113, Streinth Lab, Strasbourg University, Strasbourg, France
3 Centre of Cancer Research of Marseille (CRCM), INSERM, CNRS, Aix-Marseille Université, Marseille, France.
4 Department of Intensive Care and Thoracic Oncology, Jules Bordet Institute,Centre des Tumeurs de l’Université Libre de Bruxelles (ULB), B-1000 Brussels,Belgium.
5 Section of Computational Biomedicine, Department of Medicine, Boston University School of Medicine, Boston, MA, 02118, USA.
6 INSERM, Laboratory of Integrative Cancer Immunology, Equipe Labellisée Ligue Contre le Cancer, Sorbonne Université, Sorbonne Paris Cité, UniversitéParis Descartes, Université Paris Diderot, Université de Paris, Centre de Recherche des Cordeliers, F-75006 Paris, France.
7 Breast Cancer Translational Research Laboratory, Jules Bordet Institute,Centre des Tumeurs de l’Université Libre de Bruxelles (ULB), B-1000 Brussels,Belgium.
8 Laboratory of Molecular Immunology, Jules Bordet Institute, Centre desTumeurs de l’Université Libre de Bruxelles (ULB), B-1000 Brussels, Belgium.
9 Department of Pathology, Jules Bordet Institute, Centre des Tumeurs de l’Université Libre de Bruxelles (ULB), B-1000 Brussels, Belgium.
10 Pathology Centre, Schiltigheim, France.
11 Department of Pulmonary Medicine, CHU Saint-Pierre, Université Libre de Bruxelles (ULB), B-1000 Brussels, Belgium.
12 Laboratory of Molecular and Cellular Biology, Faculté Universitaire des Sciences Agronomiques de Gembloux (FUSAGx), B-5030 Gembloux, Belgium.
* Contributed equally to the work
† Previous affiliation for this author where the work was done partially.