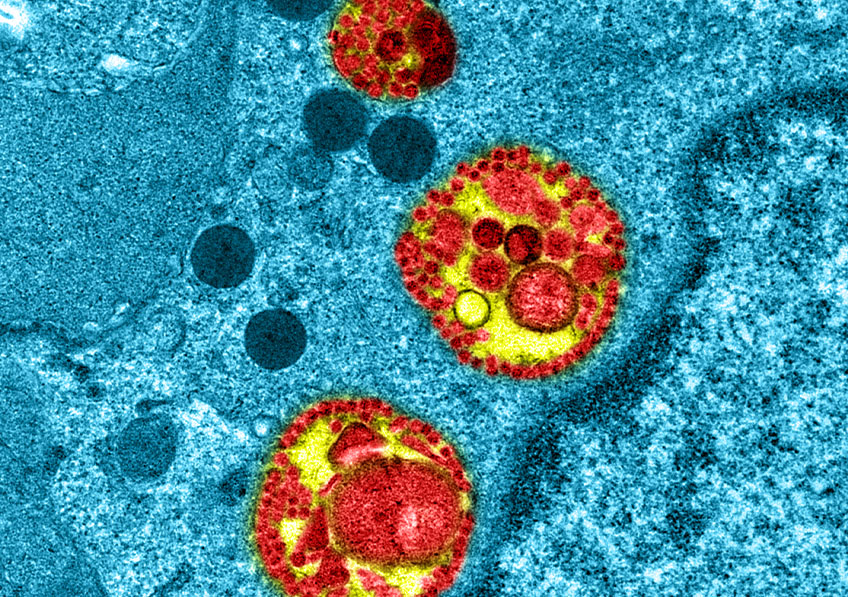
 This image shows the SARS-CoV-2 virus (in yellow). © National Institute of Allergy and Infectious Diseases – Rocky Mountain Laboratories, NIH
This image shows the SARS-CoV-2 virus (in yellow). © National Institute of Allergy and Infectious Diseases – Rocky Mountain Laboratories, NIH
Researchers from Inserm and Paris Cité University, involved in the CORIMUNO-19 study promoted by AP-HP and funded by the Fondation pour la Recherche Médicale and ANRS Maladies infectieuses émergentes (ANRS MIE), have identified biological indicators that can predict 3-month mortality in patients hospitalised for COVID-19 pneumonia. Based on two renal and one immune markers obtained from a simple blood test, combined with patients’ age, they have developed a new, simple and effective score to predict disease severity. This new tool will enable better patient care, deepen knowledge about the determinants of this infection’s severity, and help optimise clinical trials. This work also opens the door to potential avenues for other serious viral diseases. These findings are published in the Journal of Clinical Investigation Insights.
Several years after the emergence of the coronavirus pandemic and the end of the health emergency, the impact of COVID-19 continues to weigh heavily on our healthcare systems. The SARS-CoV-2 virus, which causes the infection, is still actively circulating and causing a high number of hospitalisations and even deaths. In patients, the progression and severity of COVID-19 remain difficult to determine and highly variable, ranging from asymptomatic to fatal. Until recently, it was difficult to predict which patients would develop a severe or even fatal form of the disease and therefore to focus medical efforts on those who needed it most.
This study by Inserm and Paris Cité University, sponsored by AP-HP[1] and funded in particular by the Fondation pour la Recherche Médicale and ANRS MIE, was born out of a collective effort during the first months of the pandemic. It is a game-changer, offering a new predictive tool that can inform each patient’s risk through a simple blood test. This tool was developed following the discovery by the team led by Olivia Lenoir and Pierre-Louis Tharaux, Inserm researchers at the Paris Cardiovascular Research Centre (PARCC), in collaboration with the CORIMUNO-19 consortium, of biological markers associated with higher 3-month mortality of patients hospitalised for COVID-19 pneumonia, even in moderate cases.
To identify these markers, researchers studied 196 patients admitted to 15 hospitals for moderate to severe pneumonia. Clinical samples were collected, and 41 immune mediators and markers of renal, endothelial, and vascular damage were measured in the patients’ blood within 48 hours of hospitalisation. As part of the clinical trials in which they were already participating, patients were followed for three months to precisely characterise the progression of their disease. The researchers found that age at inclusion and 14 biological variables (including 11 proteins) were independently associated with the risk of death within 90 days.
Among these, two renal markers (KIM-1, or kidney injury molecule-1, and LCN2, or lipocalin-2) and one anti-inflammatory marker (interleukin-10) proved particularly predictive of mortality. The plasma concentrations of these three markers, measured by a simple blood test, combined with patients’ age, enabled researchers to identify patients who are most at risk (2 to 3 times more likely) of fatal complications and thus to develop a new disease severity score called the “Corimuno-Score.”
Designed using a multivariate statistical model that accounts for a large number of confounding factors, this score provides maximum predictive power that rivals or surpasses most existing laboratory tests and predictors based on clinical data or imaging, which are often much more complex. These results have been replicated and validated in an independent cohort of 105 individuals.
« Numerous studies had already shown the association between certain pro-inflammatory factors and disease severity, explains Pierre-Louis Tharaux, Inserm research director and last author of this study. But very few were able to predict mortality or even to predict the risk of transfer to intensive care for these patients with initially moderate forms of the disease, as in these trials. »
This new predisposition score is a valuable tool for monitoring patients to focus efforts on those most at risk, but that’s not all. It also has scientific value, as it enables better characterisation and stratification of patients enrolled in therapeutic clinical trials, thereby making results more powerful and relevant to patients’ clinical profiles. The work also leads to a reassessment of the pathophysiology and progression of SARS-CoV-2 infection, particularly in severe forms.
« The combined predictive markers identified in this study had never before been implicated in COVID-19 outcome and reveal a whole new aspect of the disease, immune-related but also renal. It is remarkable that interleukin-10, a molecule traditionally considered anti-inflammatory, is more strongly associated with increased mortality risk than many inflammatory molecules. Similarly, the presence of KIM-1 and LCN2 indicates subclinical acute kidney injury that had previously gone unnoticed, often present despite normal kidney function. Acute kidney injury is also a major indicator of risk of death. Not all patients who die from COVID-19 show kidney damage, but this is the case for the majority of them. At this stage, however, it is impossible to say whether these lesions are the cause or the consequence of the deterioration in patients’ health, » explains Pierre-Louis Tharaux.
The study suggests that the kidney is a neglected sentinel organ in SARS-CoV-2 pneumonia and should be given greater consideration in future studies, perhaps beyond coronavirus. These findings prompt reconsideration of inter-organ interactions in sepsis, in general, and in viral sepsis[2] in particular. The identified markers may help predict the progression of other serious infectious diseases, particularly viral pneumonia such as influenza.
[1] This study is part of the Corimuno-19 consortium, promoted and funded by AP-HP, and supported by Inserm through its REACTing consortium (integrated into ANRS Emerging Infectious Diseases since January 2021).
[2] Life-threatening organ dysfunction caused by an inappropriate host response to infection.