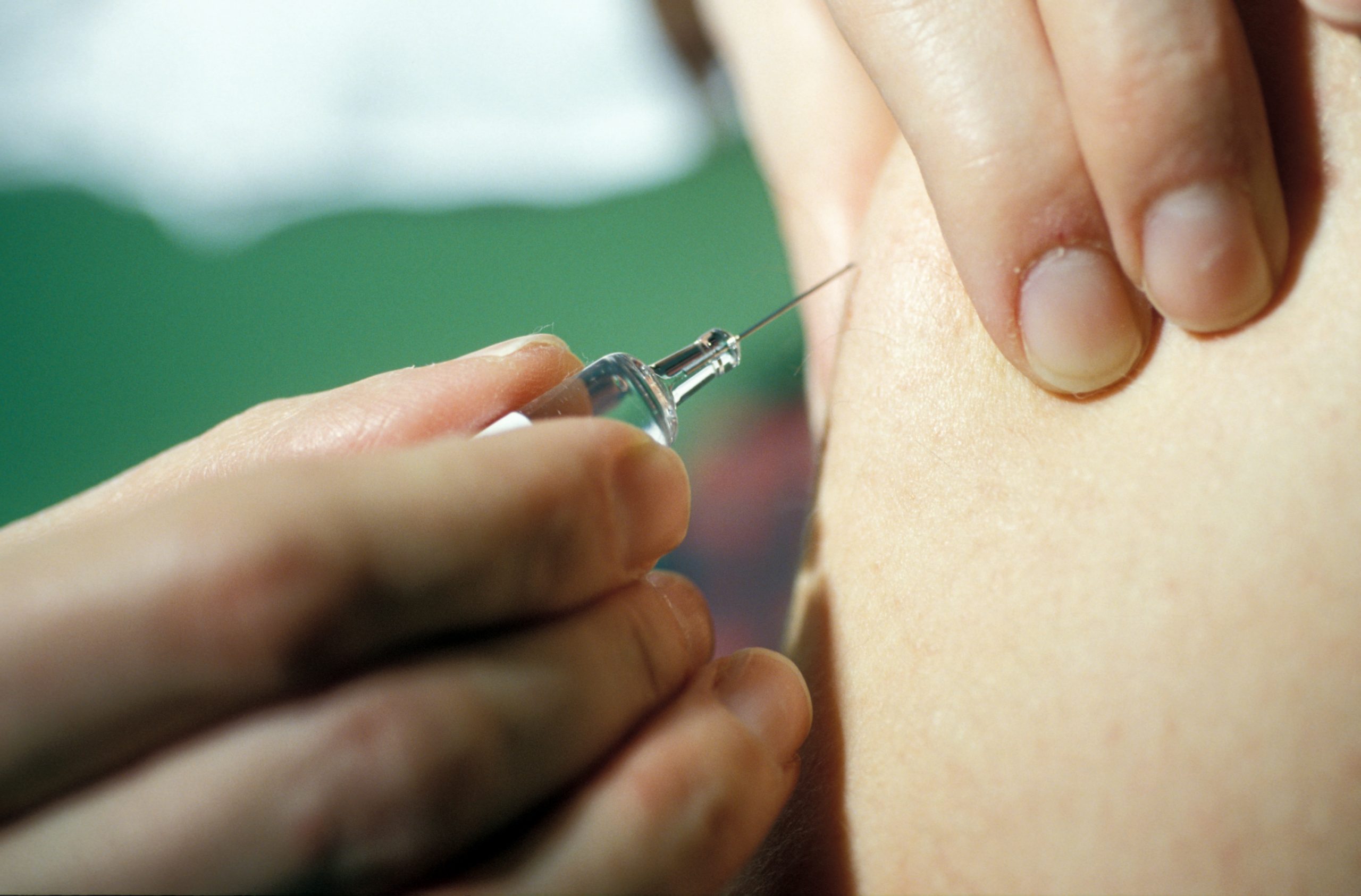
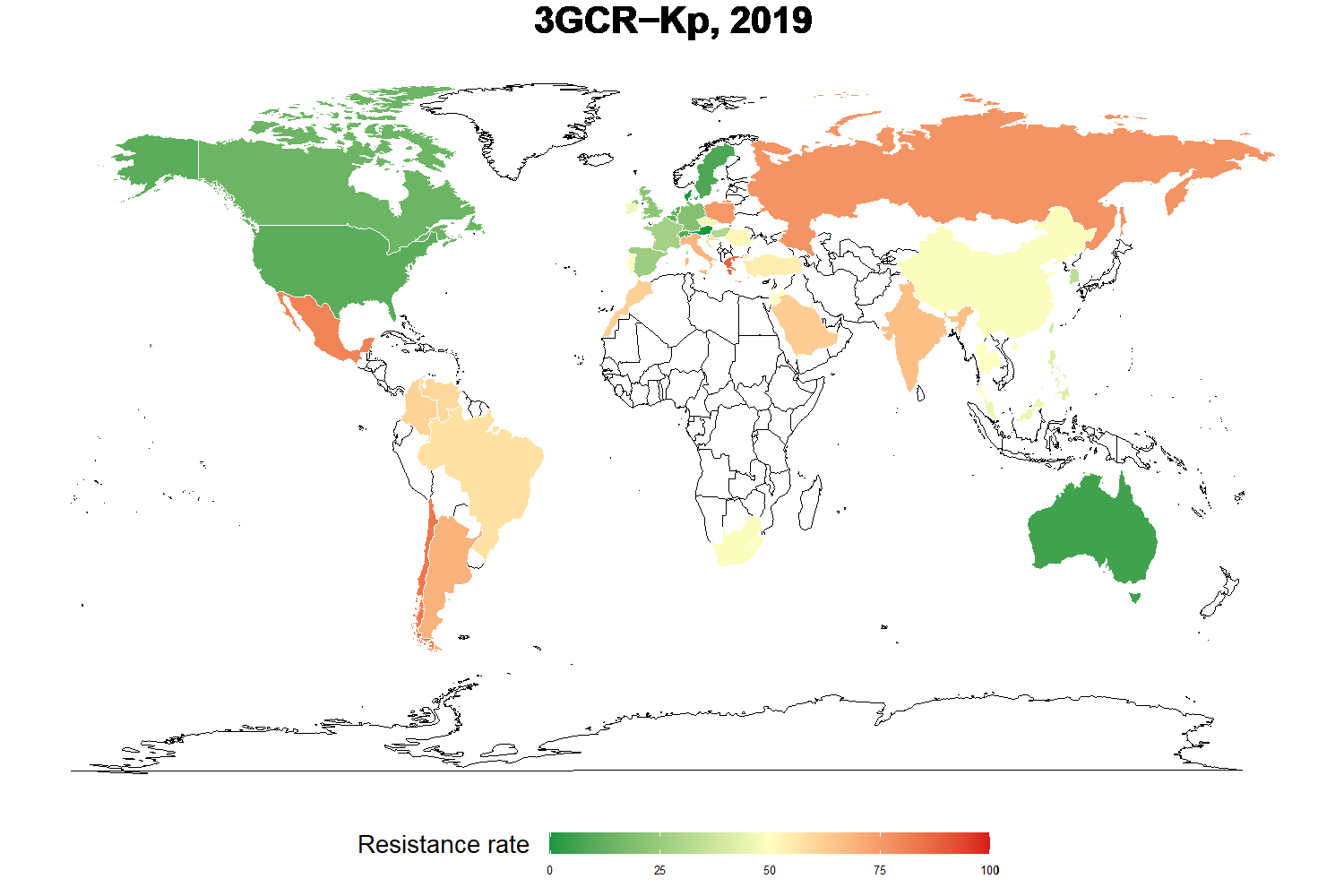
 Vaccination © Inserm/Depardieu, Michel
Vaccination © Inserm/Depardieu, Michel
The ANRS DOXYVAC trial, promoted and funded by ANRS Emerging Infectious Diseases, and conducted by research teams from Inserm, AP-HP, Université Paris Cité and Sorbonne Université (France), shows that a rapid rollout of smallpox vaccination with MVA-BN (Modified vaccine Ankara) among HIV-positive men who have sex with men significantly reduces the risk of mpox by 99%. The results of this study were published in The Lancet Regional Health-Europe on 31 July 2024.
In May 2022, cases of mpox, formerly known as monkeypox, were reported in more than 100 countries where the disease was not endemic. In France, the first case was reported on 19 May, with a rapid increase in infections among men who have sex with men (MSM).
The ANRS DOXYVAC trial, which began in 2021, was designed to study how to improve protection against sexually transmitted infections (STIs) in HIV-positive men who have sex with men.* So, when it became apparent during the course of the study that mpox cases could occur in the trial population, a smallpox vaccination was conducted, as soon as preventive vaccination in multi-partner MSM was recommended by French Health Authorities (HAS) on 11 July 2022.
To date, there is no specific vaccine against mpox. However, the virus is closely related to that of human smallpox, and the smallpox vaccine has been shown to be more than 95% effective in protecting against mpox. The vaccine used in the trial, Imvanex® (MVA-BN: Modified vaccine Ankara) from Bavarian Nordic, is a third-generation vaccine. This type of vaccine is produced from smallpox virus with the same antigens as historical smallpox. More specifically, it contains a highly attenuated form of the vaccinia virus known as “modified vaccinia virus Ankara”, a virus that does not cause disease in humans and cannot reproduce in the cells of people who are vaccinated. This means that the vaccine cannot cause local or systemic infections, particularly in immunocompromised people (such as those infected with HIV).
The aim of the analysis among participants of the ANRS DOXYVAC trial was to assess the incidence of mpox infection in participants before (9 May-10 July 2022) and after the launch of the MVA-BN vaccination campaign (from 11 July 2022), and to study the respective effects of vaccination and sexual behaviour adopted during the epidemic period on changes in incidence.
Of the 472 participants included in the analysis, 20% had been vaccinated against smallpox in childhood. The incidence rate** of mpox among trial participants, all of whom were on HIV pre-exposure prophylaxis (PrEP) and had a history of bacterial STIs, was high (49.3 per 1,000 participant-months between 9 May and 20 September 2022).
Vaccination implementation was rapid: 86% (341/398) of eligible participants had received at least one dose of MVA-BN vaccine by 20 September 2022. People were also particularly receptive to the prevention messages and recommendations, especially those with more than ten sexual partners in the last three months who are most at risk. Their sexual behaviour changed significantly before and after 9 May, leading to a reduction in the proportion of people with more than 10 partners in the last 3 months (45% compared with 38%). A significant reduction in the incidence rate of mpox was observed between the period prior to vaccination (67.4 per 1,000 months between May 9 and July 10, 2022) and the period following the launch of the vaccination campaign (24.4 per 1,000 months between July 11 and September 20, 2022).
This trial demonstrated that the rapid implementation of smallpox vaccination with MVA-BN in MSM undergoing PreP significantly reduced the risk of mpox, with an estimated 99% reduction in incidence between the two periods. The reduction in risky sexual behaviour among those most at risk also probably contributed to the reduction in incidence, but to a lesser extent than the vaccination programme.
This study emphasises that identifying and prioritising at-risk populations, delivering targeted prevention messages and awareness campaigns, ensuring the availability of a smallpox vaccine and, above all, the rapid rollout of vaccination to people at risk should enable health authorities to control a future mpox epidemic like the one that occurred in 2022.
* DOXYVAC has demonstrated the efficacy of post-exposure doxycycline in reducing the occurrence of chlamydial infections, syphilis and, to a lesser extent, gonococcal infections.
** Incidence is the number of new cases of a disease in a year in a given population (not to be confused with prevalence, which refers to the number of sick people at a given time). The incidence rate of a disease corresponds to the number of individuals having contracted a disease per 1,000 people exposed to the risk of this disease (in the DOXYVAC trial, it is calculated for one month) (https://www.ined.fr/en/glossary/incidence-of-a-disease/).