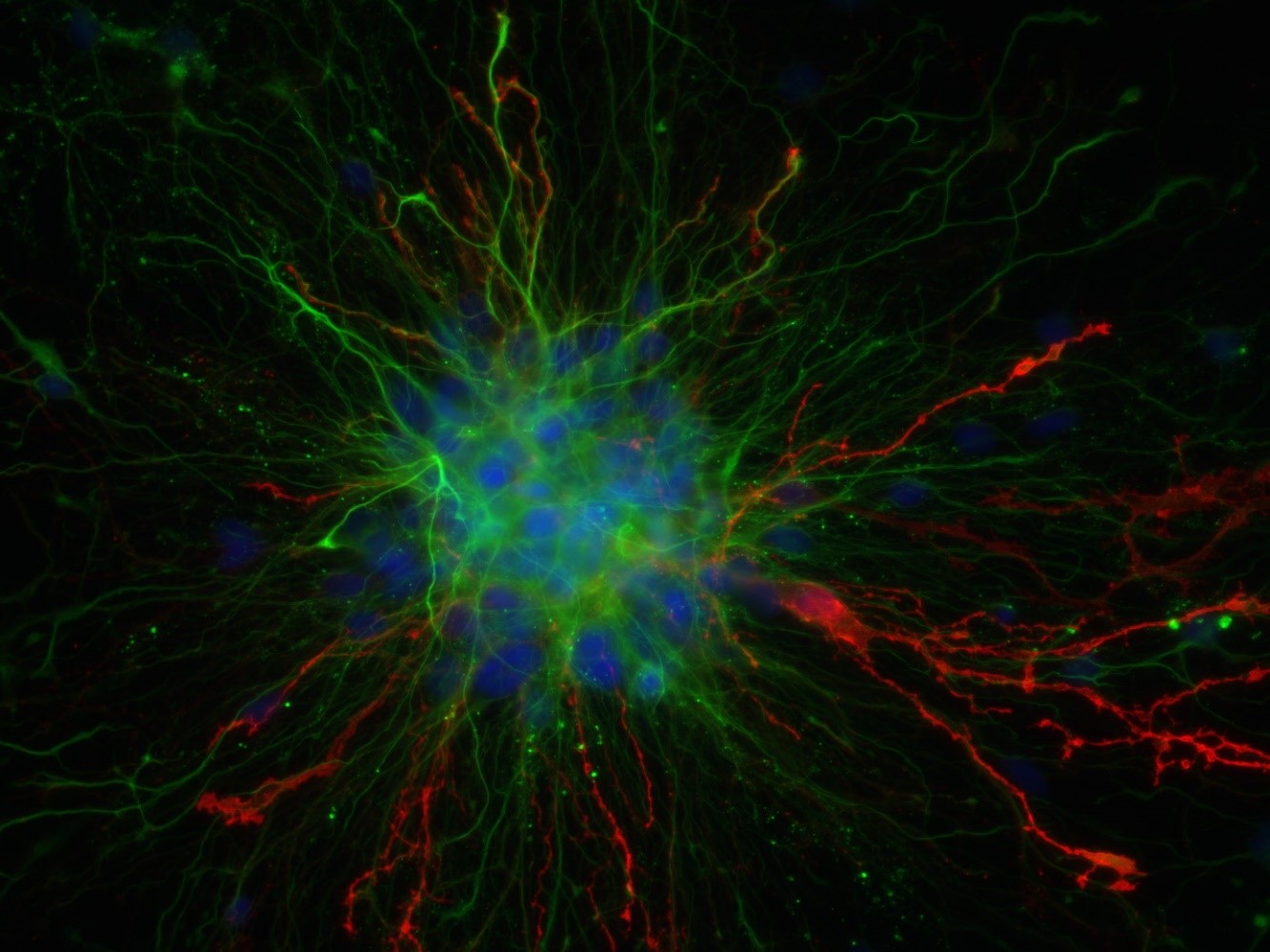
Glioblastomas are the most common tumors of the central nervous system Image taken using a Zeiss Axioimager Z1 widefield epifluorescence microscope. Inserm/Guichet, Pierre-Olivier
Glioblastomas are the most common type of brain tumor, and their prognosis is often highly unfavorable. A collaborative study by Jean-Léon Thomas, Inserm researcher at the Brain & Spine Institute (Inserm/CNRS/Sorbonne Université) and Pitié-Salpêtrière Hospital AP-HP, and Akiko Iwasaki (Department of Immunology, Yale University School of Medicine, USA), has revealed the beneficial role played by the meningeal lymphatic vascular network in treating these tumors – in the short and longer term. Their findings have been published in Nature.
Glioblastomas are not just the most commonly occurring type of brain tumor, they are also the most severe. With an estimated prevalence of 1/100,000, they mainly affect patients between 45 and 70 years of age. Treatment currently involves surgery combined with radiation therapy and chemotherapy. Therapeutic benefit, in terms of survival, remains modest (currently around 18 months), inciting researchers to continue to explore new avenues of potential treatment.
Eric Song (Yale University), first author of this study, Jean-Léon Thomas, Akiko Iwasaki and their colleagues studied the meningeal lymphatic network to see whether it regulates the immune system in response to the presence of a brain tumor. A veritable pipework of lymphatic vessels in the meninges surrounding the brain, the meningeal lymphatic network has been generating particular interest since the publication of studies over the previous five years showing its connection to the lymph nodes of the neck (where immune cells proliferate and differentiate), and its role of draining immune cells into the latter.
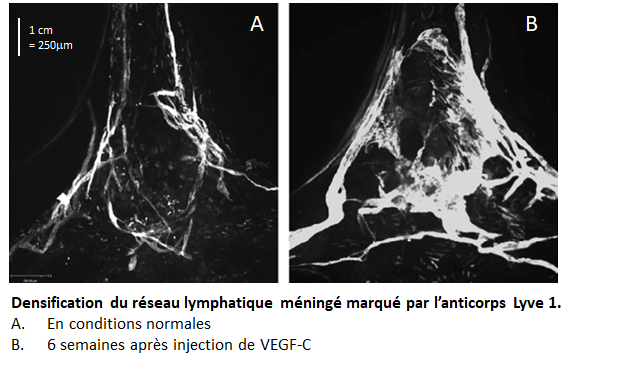
In their latest study, published in Nature, the researchers worked with animal models of glioblastoma. They showed that the tumor would disappear following prior enlargement of the meningeal lymphatics – achieved by injecting the meninges with lymphatic growth factor VEGF-C. The growth of the meningeal lymphatic network induced by VEGF-C (as can be seen in the photo) was correlated with the mass entry of immune T cells (CD4 and CD8), which under normal conditions are absent, into the tumor environment.
This short-term response destroys the tumor and is accompanied by the persistence of “memory cells” specifically directed against the tumor cells, which makes it possible to reject the same tumor in the longer term.
Nevertheless, the researchers’ experiments show that it is in combination with an immunotherapy already used in neuro-oncology that the transient VEGF-C treatment is the most effective, enabling complete eradication of the existing glioblastoma. “Our study highlights the fact that reinforcing the network of meningeal lymphatic vessels increases tumor antigen traffic from the meninges to the lymph nodes”, explains Thomas.
With his colleagues, he concludes that the major role of this network is to transport, from the meninges, an immune alert message triggering activation of the lymphocytes directed against the tumor.
The findings of this study therefore open up new avenues in the treatment of brain tumors by targeting the meningeal lymphatic vessels and their associated lymph nodes.
The researchers wish to continue their work by studying the role of the meningeal lymphatic network in other diseases. “We are currently exploring the functional mechanisms and therapeutic potential of this vascular network with novel experimental models, and in other nervous system diseases – neurodegenerative, neurovascular and infectious“, concludes Thomas.These contents could be interesting :
VEGF-C-driven lymphatic drainage enables brain tumor immunosurveillance
Eric Song1, Tianyang Mao1, Huiping Dong1, Ligia Simoes Braga Boisserand2, Salli Antila5, Marcus Bosenberg1,3,4, Kari Alitalo5, Jean-Leon Thomas2,6,8*, Akiko Iwasaki1,3,7,8* 1 Department of Immunobiology, Yale University School of Medicine, New Haven, CT, 06520, USA. 2 Department of Neurology, Yale University School of Medicine, New Haven, CT, 06520, USA. 3 Department of Dermatology, Yale University School of Medicine, New Haven, CT, 06520, USA. 4 Department of Pathology, Yale University School of Medicine, New Haven, CT, 06520, USA. 5 Translational Cancer Medicine Program and Wihuri Research Institute, Biomedicum Helsinki, University of Helsinki, FIN-00014, Helsinki, Finland 6 Institut du Cerveau et de la Moelle Épinière, INSERM U1127, CNRS UMR 7225, GH Pitié-Salpêtrière, Sorbonne Université, 75013 Paris, France 7 Howard Hughes Medical Institute, Chevy Chase, MD, 20815, USA 8 These authors jointly supervised this work: Jean-Leon Thomas, Akiko Iwasaki
DOI : 10.1038/s41586-019-1912-x
VEGF-C-driven lymphatic drainage enables brain tumor immunosurveillance
Eric Song1, Tianyang Mao1, Huiping Dong1, Ligia Simoes Braga Boisserand2, Salli Antila5, Marcus Bosenberg1,3,4, Kari Alitalo5, Jean-Leon Thomas2,6,8*, Akiko Iwasaki1,3,7,8*
1 Department of Immunobiology, Yale University School of Medicine, New Haven, CT, 06520, USA.
2 Department of Neurology, Yale University School of Medicine, New Haven, CT, 06520, USA.
3 Department of Dermatology, Yale University School of Medicine, New Haven, CT, 06520, USA.
4 Department of Pathology, Yale University School of Medicine, New Haven, CT, 06520, USA.
5 Translational Cancer Medicine Program and Wihuri Research Institute, Biomedicum Helsinki, University of Helsinki, FIN-00014, Helsinki, Finland
6 Institut du Cerveau et de la Moelle Épinière, INSERM U1127, CNRS UMR 7225, GH Pitié-Salpêtrière, Sorbonne Université, 75013 Paris, France
7 Howard Hughes Medical Institute, Chevy Chase, MD, 20815, USA
8 These authors jointly supervised this work: Jean-Leon Thomas, Akiko Iwasaki
DOI : 10.1038/s41586-019-1912-x

