
Obesity is a global public health problem whose incidence continues to increase. According to the World Health Organization (WHO), the number of cases worldwide has almost tripled since 1975.
Obesity is associated with many comorbidities and has a high rate of mortality. This complex chronic disease is therefore estimated to increase the risk of cardiovascular disease (the leading cause of death worldwide), diabetes, musculoskeletal disorders, many forms of cancer (endometrial, breast, ovarian, prostate, liver, gallbladder, kidney, colon, etc.). More recently, data have shown that people with obesity are more susceptible to severe forms of COVID-19. Its impact on population health and its economic and social costs are therefore considerable.
This major public health issue is also one that affects France. In order to evaluate the impact of preventive measures such as the country’s National Nutrition and Health Program (PNNS), it was important to take thorough stock of the current epidemiological situation. The latest study on the subject, on the initiative of the French League Against Obesity and coordinated by researchers from Inserm and Montpellier University Hospital, was published in February in the Journal of Clinical Medicine. Based on the figures collected by the Odoxa polling institute, this study reveals the extent of the problem in highlighting that 47.3% of French adults are obese or overweight. It also provides specific information on the most affected populations by age group, region and socioprofessional activity, making it possible to refine prevention policies.
And beyond these prevention measures that are crucial to fighting obesity, how can we support individuals who are overweight or obese? While lifestyle interventions, particularly diet and physical activity, are essential, appropriate management is based on multidisciplinary and personalized approaches that also incorporate solutions in the form of medication, surgery, or both. Much progress has been made in recent years in the field of medication, as described in a literature review published in The Lancet, to which contributed Karine Clément, professor of nutrition and director of the Inserm unit Nutrition and Obesities: Systemic Approaches (Nutriomics).
Overweight and Obesity: Definition Elements
Obesity is defined by excessive body fat and modification of the adipose tissue, which cause health problems and can reduce life expectancy. Its causes are complex. It is the result of several factors – dietary, genetic, epigenetic and environmental – that come together and influence the development and progression of this chronic disease.
Adults are considered to be overweight when their body mass index (BMI) is equal to or greater than 25 and obese when their BMI is equal to or greater than 30. For children, age must be taken into account when defining overweight and obesity.
Read our special feature on obesity (only available in French).
The Latest Figures for France
Obépi-Roche is the name given to a series of surveys which had been coordinated by Inserm every three years between 1997 and 2012 in order to produce estimates of overweight and obesity prevalence in France. A new edition of this survey was launched by the French League Against Obesity in 2020, based on questionnaires collected by the Odoxa polling institute on a sample of 9 598 people living in mainland France, aged 18 years or older, and built using the quota-sampling method[1]. Coordinated by Annick Fontbonne, researcher at Inserm and David Nocca, doctor at Montpellier University Hospital, the analysis of the results reveals a worrying situation.
It showed that the prevalence of excess weight (which includes both overweight and obesity) was 47.3%, with 17% of subjects being obese. At first glance, these figures do not appear to be very different from the last estimates of the Obépi-Roche study of 2012. However, if we bear in mind the trends since 1997 and consider overweight and obesity separately, the observation is less favorable.
Since 1997, the prevalence of overweight has always fluctuated at around 30%, whereas that of obesity has continued to rise rapidly, from 8.5% in 1997 to 15% in 2012, and then to 17% in 2020. This increase is even more marked in the youngest age groups and for morbid obesity, whose prevalence had multiplied by around seven over the period.
“So we have to note that contrary to the expectations of public authorities and health professionals alike, obesity in France has continued to grow year on year since the rollout of the PNNS in 2001,” emphasize Annick Fontbonne and David Nocca.
The researchers went further in the analysis by highlighting differences in prevalence according to sex and age, region, and socioprofessional category.
Sex and Age
Older people are more overweight or obese than their younger counterparts, with excess weight affecting 57.3% of people aged 65 years and over compared to 23.2% of 18-24-year-olds. Nevertheless, the trends are more worrying, given that the youngest age groups have had the highest prevalence of obesity over the years. Since 1997, obesity among the 18-24-year-olds has more than quadrupled, and has almost tripled among the 25-34-year-olds, while the increase among those aged 55 and older has been low since 2009.
Differences between the sexes have also been observed. In 2020, while men were more often overweight than women (36.9% vs. 23.9%, respectively), the opposite was the case for obesity (16.7% vs. 17.4%, respectively).
 Evolution of the prevalence of obesity by age groups between the 1997-2012 Obépi-Roche surveys and the 2020 Obépi survey.
Evolution of the prevalence of obesity by age groups between the 1997-2012 Obépi-Roche surveys and the 2020 Obépi survey.
Regional Disparities
The prevalence of obesity in 2020 exceeds 20% in north and northeastern France, and is the lowest (below 14.5%) in Île-de-France and Pays de la Loire. If we exclude the latter two regions and Brittany, we see a decrease in the prevalence gradient when moving from the northern to the southern regions of France.
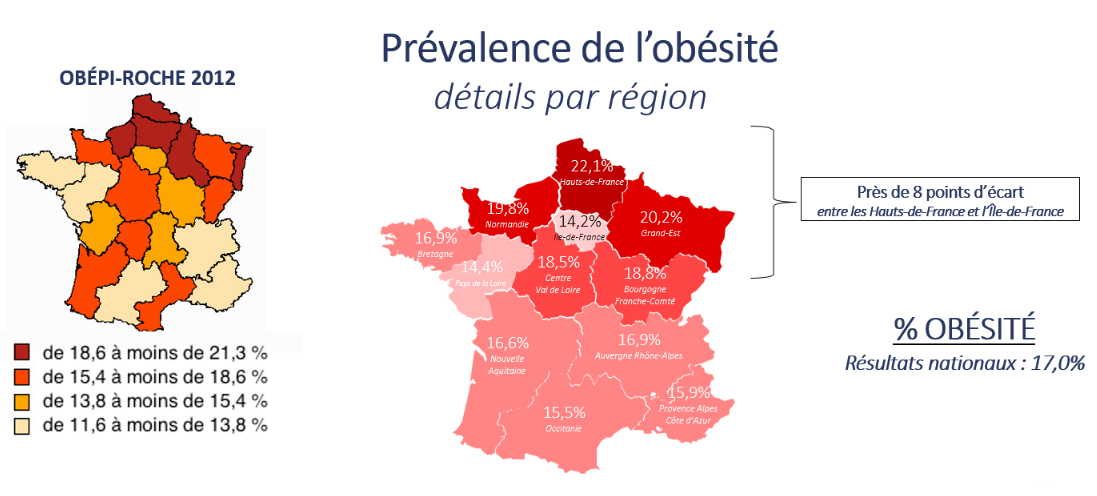 Geographic distribution of the prevalence of obesity in 2020 in the French regions
Geographic distribution of the prevalence of obesity in 2020 in the French regions
Socioprofessional Categories
The scientific literature reveals that overweight and obesity are generally more common in the disadvantaged social categories. The Obépi 2020 study confirms this observation for the occupational qualification criterion, as the prevalence of excess weight is 51.1% among factory workers or equivalent, 45.3% among clerks, 43% among people in intermediate jobs, and 35% among managers or people in equivalent positions.
The trend is the same when we look at obesity: while the figures are similar for factory workers or equivalent (18%) and clerks (17.8%), they are markedly lower among managers or people in equivalent positions (9.9%). The intermediate jobs have a prevalence of obesity of 14.4%. It should also be noted that the trends have been increasing since 1997 in all occupational categories.
The authors conclude: “The study had been much awaited in order to obtain a rigorous overview of overweight and obesity in France. When compared to previous surveys, it has shown that although the prevalence of excess weight (overweight and obesity) is appearing to plateau, the prevalence of obesity is increasing rapidly and has doubled since 1997. In addition, the slope is more pronounced in younger generations and for the most severe degrees of obesity. Given the slight differences in methodology between the 1997-2012 and 2020 surveys, it would be desirable to repeat this series of surveys in order to confirm and monitor these worrying trends. “
Managing Obesity: Innovative Multidisciplinary Approaches
While prevention is the cornerstone in the fight against obesity and its associated comorbidities, it is also necessary to recognize that it is a complex chronic disease, to which therapeutic responses should also be provided.
The goal of obesity management is to improve health. Sustained weight loss of more than 10% overall bodyweight improves many of the complications associated with obesity (e.g. prevention and control of type 2 diabetes, hypertension, fatty liver disease, cardiovascular diseases and obstructive sleep apnea), as well as quality of life.
However, maintaining the weight loss is the major challenge of obesity management. Like all complex chronic diseases, obesity depends on factors that vary from one individual to another and managing it requires a long-term, multimodal approach, taking into account each individual’s treatment goals, and the benefits and risks of the different therapies.
Lifestyle interventions (dietary habits, physical activity/inactivity, sleep, psychological difficulties, etc.) form the first pillar of this management, but they are rarely sufficient in achieving and maintaining significant long-term weight loss. Depending on individual situations, management can therefore be combined with other strategies that include anti-obesity medications and bariatric surgery.
Medication
Most available “historical” anti-obesity medications work on neurotransmitters (such as serotonin) that act on appetite regulation and reward circuits, in order to reduce hunger, promote the feeling of satiety, and decrease the reward sensation associated with food. Many of these treatments have had to be withdrawn due to side effects, leaving patients and their doctors without pharmacological tools.
However, over the past five years, significant therapeutic advances have led to the development of a new generation of anti-obesity medications. These new treatments, which are similar to the intestinal hormones (incretins) and also used in combination with other molecules (GLP1, GIP, etc.), are highly effective. They are associated with weight losses of more than 10% of overall bodyweight in more than two-thirds of clinical trial participants. Known for their initial actions on the pancreas by promoting the secretion of insulin, they also act on satiety mechanisms in the central nervous system. Long-term data on safety, efficacy, and cardiovascular outcomes are awaited in order to make progress in bringing these medications to market.
These advances also concern a new targeted treatment for rare and very severe forms of genetic obesity that begin in childhood. This treatment induces weight loss by acting on the serious eating disorders experienced by these patients and leads to an improvement in their quality of life and that of those around them.
And What About Surgery?
Long-term studies have shown that bariatric surgical procedures typically lead to a durable weight loss of 25% and rapid, sustained improvements in complications of obesity and in mortality. Less invasive endoscopic techniques are also possible in some cases. However, the surgical approach, more invasive than medication, has not yet been compared to the new-generation anti-obesity treatments.
“Further work is required to determine optimal patient-specific treatment strategies, including combinations of lifestyle interventions, anti-obesity medications, endoscopic and bariatric surgical procedures, and to ensure equitable access to effective treatments for these complex pathologies,” concludes Clément, co-author of the literature review published in The Lancet.
[1]The quota method is a sampling method that consists of ensuring the representativeness of a sample by assigning it a structure similar to that of the general population.
These contents could be interesting :
Prevalence of Overweight and Obesity in France: The 2020 Obepi-Roche Study by the “Ligue Contre l’Obésité”
Annick Fontbonne1,2,* , Andrew Currie3,4, Patrick Tounian5 , Marie-Christine Picot1,6 , Olivier Foulatier7, Marius Nedelcu8,9 and David Nocca 4,10
1 Centre of Clinical Investigation, Inserm, Montpellier University Hospital, 34295 Montpellier, France
2 Centre for Epidemiology and Population Health, Inserm, Paris-Saclay University, USQV, 94805 Villejuif, France
3 Department of Upper GI Surgery, Epsom & St Helier NHS Trust, Epsom KT18 7EG, UK
4 Saint Eloi Hospital, Montpellier University Hospital, 34295 Montpellier, France
5 Pediatric Nutrition and Gastroenterology Department, Trousseau Hospital, APHP, Sorbonne University, 75571 Paris, France
6 Clinical Research and Epidemiology Unit (Department of Medical Information), Inserm, Montpellier University Hospital, 34295 Montpellier, France
7 Scientific Council, “Ligue Contre l’Obésité” (League Against Obesity), 75008 Paris, France
8 ELSAN, Saint Michel Clinic, Surgical Centre for Obesity, 83100 Toulon, France
9 ELSAN, Bouchard Clinic, 13006 Marseille, France
10 Institute for Functional Genomics, UMR 5023 CNRS-U1191, Inserm, Montpellier University, 34295 Montpellier, France
*Author to whom correspondence should be addressed.

