It is well known that breast feeding increases the secretion of the prolactin hormone and inhibits ovulation in women. This prevents the onset of a new pregnancy too soon, and so breast feeding was used in the past as a method of contraception. In addition to this physiological condition, there are many other pathological conditions in which the production of prolactin is increased. One of the most frequent is the existence of tumours that induce an over-secretion of this hormone. These women present with chronic infertility due to anovulation. Thanks to the work of the Inserm researchers from unit 693 “Steroid receptors: endocrinian and metabolic physiopathology”, the intimate mechanism of the hyperprolactinaemia alterations affecting reproduction in mice has been discovered.
This work has been published in the journal JCI.
Hyperprolactinaemia is a major cause of anovulation and is responsible for menstruation disorders and infertility. However, not much was know in detail of the mechanisms that cause this pathology.
All that was known was that an increase in prolactin in women disturbed one of the most important hormones affecting reproduction and fertility: GnRH[1].
Up until now, we had been unable to understand this inhibition of prolactin in the GnRH neurons, because most of these neurons did not express the prolactin receptor.
So the researchers put forward another hypothesis: what if it was due to the indirect action of other molecules?
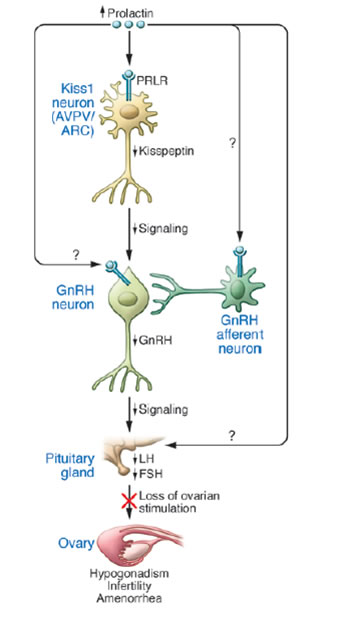
The team led by Jacques Young and Nadine Binart from Inserm unit 693 “Steroid receptors: endocrinian and metabolic physiopathology” at the Bicêtre hospital, discovered that prolactin had an indirect effect on GnRH. Using mice as models, they demonstrated that prolactin effectively inhibits the secretion of neurons situated upstream the GnRH neurons and that are essential to their functioning. They secrete a neurohormone known as kisspeptin.
Kisspeptin: the key to infertility?
In mice, hyperprolactinaemia directly inhibits the secretion of kisspeptin and by preventing the secretion of GnRH, effectively blocks ovarian cyclicity. By administering kisspeptin, we can restore the release of GnRH and restart ovarian cyclic functioning and ovulation despite hyperprolactinaemia.
The effect of hyperprolactinaemia on the ovulation cycle (credit: J Young/Inserm)
This is both a physiopathological discovery that for the first time explains the link between infertility and hyperprolactinaemia, and a new approach opening the way to an original therapy. On-going studies are aiming to validate the concept in women, so that we can provide a therapeutic alternative when the subject is resistant to the available medication.
[1] GnRH is a hypothalamic hormone released in a pulsatile manner. It regulates what is known as the pituitary gonadotropins LH and FSH that control ovarian cyclicity
These contents could be interesting :
Hyperprolactinemia-induced ovarian acyclicity is reversed by kisspeptin administration
Charlotte Sonigo, 1 Justine Bouilly,1 Nadège Carré,1 Virginie Tolle,2 Alain Caraty,3 Javier Tello,4 Fabian-Jesus Simony-Conesa,4 Robert Millar,4,5,6 Jacques Young,1,7 and Nadine Binart1,7
1INSERM U693, Université Paris-Sud, Faculté de Médecine Paris-Sud, Le Kremlin-Bicêtre, 2INSERM U894, Centre de Psychiatrie et Neurosciences,Université Paris Descartes Sorbonne Paris, Paris, France. 3UMR 6175 INRA–CNRS–Université Tours, Nouzilly, France. 4Centre for Integrative Physiology, University of Edinburgh, Edinburgh, United Kingdom. 5Mammal Research Institute, University of Pretoria, Pretoria, South Africa. 6UCT/MRC Receptor Biology Unit, University of Cape Town, Cape Town, South Africa. 7Assistance Publique–Hôpitaux de Paris, Service d’Endocrinologie et des Maladies de la Reproduction, Hôpital Bicêtre, Le Kremlin Bicêtre, France.
Journal of Clinical Investigation octobre 2012