The European EUCelLEX Project (Cell-based regenerative medicine: new challenges for EU legislation and governance), coordinated by Inserm for a three-year period, funding to the tune of €500,000 from the European Union. The project consists in a full examination of the application of the European rules regarding cell banks together with current practices in respect of the therapeutic use of human cells in the different countries concerned. The purpose is to submit the data obtained to the European Commission for it to draw up legislative measures in line with medical advances in this field. On 4 December the nine research teams in Europe and Canada met at the Political Sciences Research Centre in Paris (CEVIPOF) for the launching of the project.
Biobanks: the future of regenerative medicine
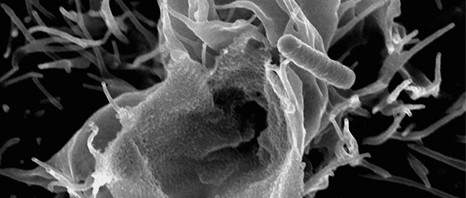
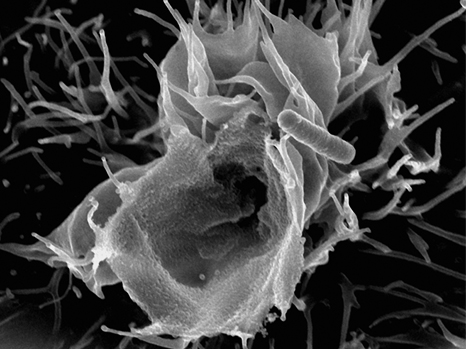
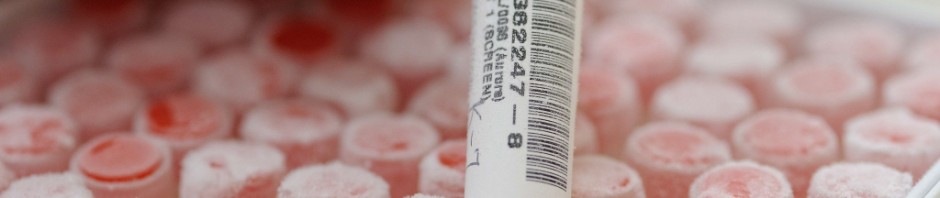
Today, human biological specimens are seen as resources essential to advances in the life sciences and medicine. The analytical data obtained enable a better understanding of the various diseases and also make it possible to propose the appropriate treatment, notably in the field of regenerative medicine[1]. Gathering, storing, processing and distributing them are all done by the biobanks – key players in the transfer of scientific knowledge to clinical practice. These biological databanks will enable researchers to identify new clinical biomarkers and develop new therapeutic approaches such as regenerative medicine. In this field, research into stem cells continues to be promising, stimulating as it does the body’s self-healing ability.
Need for a legal definition of the use of human biological specimens at European level
From 2004 to 2006, the European Union adopted three directives governing cells and human tissues in order to standardise their acquisition, their storage and their use for therapeutic purposes. These directives apply specifically to tissue and cell banks, including cord blood strains and cells used for regenerative medicine. However, they were used in very different ways from one country to another. “At present, the European legal texts concerning the use of stem cells for research by the players in the public and private sectors are not such as to enable the efficient sharing of these resources in Europe, which may impede advances in research,“ explains Emmanuelle Rial-Sebbag, coordinator of the EUCelLEX Project.
Furthermore, scientific developments in the use of human cells centre around new legal and institutional issues. More particularly, the development of research infrastructures at European level (BBMRI-ERIC, FCrin[2]) means re-examining the relevance of all this in the light of rapidly expanding clinical practice which also has to take public health issues into account. Thus today, the areas of examination can be seen to be expanding, and hence the inadequacy of European legislation regarding cell research. It should added that certain parts of the process of translating basic knowledge, up to and including the marketing of new products, are unequally regulated, either by the national laws of the member states or by Europe.
The EUCelLEX Project objectives
It is within this context that the EUCelLEX Project’s chief objective is to examine current legislation concerning the therapeutic use of somatic cells, in both the public and private sectors and in a number of European countries.
To this end, the project aims to assess the relevance of current European legislation in order to provide the data needed to establish a European framework for the use of stem cells of every type (embryo, adult and IPS cells from cord blood) in the light of recent scientific, legal and institutional developments in Europe. To obtain a complete picture of the European situation, the legal study will be complemented by an examination of current clinical practices together with the many ethical recommendations throughout Europe. Starting with the observation that the entire translational process, from research to the marketing of a product, is only partially covered by the EU rules, the teams will need to examine the heterogeneous nature of the legislation due to the freedom of action allowed to the member states.
Initially, each of the partners in the project will need to examine the legislation and the policies in their respective countries governing the use of stem cells at both national and European level.
They will then compare current legislation with the practices that are due to develop stem cells in the near future, more especially in the research infrastructures to highlight the deficiencies and propose sustainable solutions. Special interest will also be paid to emerging such as “cell tourism” or the use of unproved therapies. For example, in some European countries doctors propose to use regenerative medicine techniques which have yet to be scientifically validated and which do not meet the safety criteria imposed by both French and European legislation.
The ultimate objective is to make recommendations to the European Commission so as to facilitate the use of stem cells for clinical purposes in a stabilised legal context.
Thus the results of the project will enable innovation in research and help the European to implement specific legislation in this field.
The 4 phases of the EUCelLEX Project:
1. Information gathering on the legal implementation of the directive on tissues and cells, with the focus on current European legislation and the regulations set forth at national level.
2. Integration of this knowledge into a wider analytical context covering the entire field, focusing on stem cells and the cord blood banks.
3. Make an in-depth analysis of the legislation, the literature, case law and the gathering of opinions on the various ethical aspects.
4. Create tools for the participation of the professional people involved and he key players in the questions raised by the use of stem cells.
The research partners in the EUCelLEX consortium, based throughout Europe and in Canada, will use their scientific, legal and ethical skills to highlight the issues raised by the use of stem cells for the medicine of tomorrow.
EUCelLEX – Cell-based regenerative medicine: new challenges for EU legislation and governance
(Reference : 601806)
The EUCelLEX Project is to be launched on 4 December 2013 and will be aided by the European Union (FP7) for a period of three years. It is coordinated by Inserm and involves nine partners based in seven European countries and Canada:
Inserm (coordinator), France: http://www.inserm.fr/
Leibniz University, Germany: http://www.uni-hannover.de/en/index.php
Central European University, Budapest, Hungary: http://www.ceu.hu/
Legal Pathway, Netherlands
Oxford University, England: http://www.oP.ac.uk/
Medical University of Graz, Austria: http://www.meduni-graz.at/en/
National Political Sciences Foundation, France: http://www.sciencespo.fr/
KU Leuven, Belgium: http://www.kuleuven.be/english/
McGill University, Canada: http://www.mcgill.ca/fr
[1] Regenerative medicine is a multidisciplinary field of research whose clinical applications are based on the repair, replacement or regeneration of cells, tissues or organs in order to restore an impaired function, irrespective of the cause, including congenital anomalies, diseases, traumas and ageing. It uses a combination of several technological approaches designed to replace traditional grafts.
[2] Biobanking and Biomolecular Resources Research Infrastructure – European Research Infrastructure Consortium, French Clinical Research Infrastructure Network