The Ebola epidemic is continuing to spread across West Africa. In March 2014, Guinea notified its first cases of Ebola virus illnesses to the World Health Organisation (WHO). Since then it has spread across borders, to Liberia, Sierra Leone and Nigeria.
According to the latest WHO report, dated 18 September, 5 762 cases of Ebola have been identified and 2 793 people have died.
What is Ebola virus?
Ebola virus is a highly contagious, fatal virus. After 2 to 21 days incubation, the disease appears as non-specific symptoms (fever, tiredness, muscle and joint pain) before developing into a phase characterised by gastro-intestinal signs such as bloody diarrhoea, vomiting, respiratory and sometimes neurological symptoms. In 40% to 80% of cases, the development is fatal.
Researchers at Inserm (the P4 Laboratory in Lyon) and the Pasteur Institute revealed, in an article published last April in The New England Journal of Medicine, using samples originating from Guinea, that the virus currently spreading in West Africa is actually a variant of the Ebola virus identified in the Republic of Congo and the Gabon. In fact, the analysis showed only 97% similarity with strains sampled in these two countries. The remaining 3% therefore demonstrate that it is a new ‘form’ of the Ebola virus in Guinea.
How is Ebola virus research organised at Inserm?
- The International Centre for Infectiology Research (CIRI)
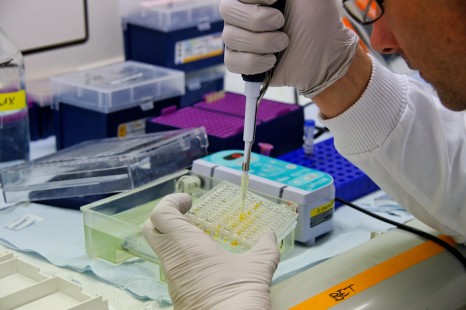
The CIRI (a mixed unit created on 1st January 2013 by Inserm, CNRS, ENS Lyon and University Claude Bernard Lyon 1) brings twenty scientific teams together with a common objective: to better understand and control infectious diseases, such as the Ebola virus. It has become a very important player in fundamental, diagnostic and therapeutic research in a number of fields (including virology, bacteriology and immunology).
CIRI is the only research centre in France involved in the study of this type of viral haemorrhagic fever. Four of its teams are currently researching the latter at the P4 Inserm-Jean Mérieux laboratory. These teams are “Unit of Biology for Emerging Viral Infections”, “Molecular Basis of Viral Pathology”, “Enveloped Viruses, Vectors and Innate Responses” and “Cell Biology of Viral Infections”.

The International Centre for Infectiology Research (Inserm Unity 1111) ©Inserm/Guénet, François
Inserm Research Director Vincent Lotteau and his team (“Cell Biology of Viral Infections”) were recently entrusted with such a research project concerning the Ebola virus. Their work generally involves the identification of cellular functions that are used by viruses to replicate.
In particular, Vincent Lotteau and his team have created a unique systems biology platform at the Lyonbiopôle Centre of Infectiology. With its thorough knowledge on how viruses perturb cell host functions, the platform can investigate protein interaction networks and identify new therapeutic targets and molecules. This year, Vincent Lotteau and his colleagues created the start-up Enyo Pharma to conduct initial proofs of concept for this approach on the flu virus and hepatitis B.
Through the initiative of the Institute of Microbiology and Infectious Diseases (IMMI), Vincent Lotteau’s team and Enyo Pharma are currently working on the identification of drugs that already have marketing authorisation and could be repositioned for therapeutic indications against Ebola. Once these molecules are identified, they will be tested in vivo and in vitro at the P4 Inserm-Jean Mérieux laboratory.
- The Jean Mérieux-Inserm P4 laboratory
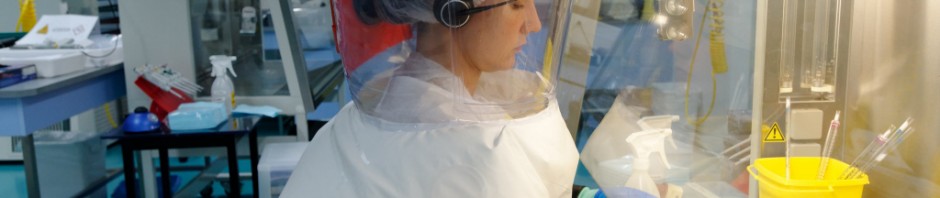
The Jean Mérieux-Inserm P4 laboratory is a high-level containment laboratory dedicated to the study of Class 4 pathogens. The biological safety level applied is 4, the highest possible level. The researchers working there wear a full body, air-supplied, positive pressure suit to protect them from all contamination. The laboratory is itself maintained under negative pressure in order to protect the environment. Moreover, all wastes produced are completely inactivated, and the exhaust air is purified by a double absolute filtration system. This laboratory today remains the structure offering the largest experimental capacity in Europe for this containment level.

The Jean Mérieux-Inserm P4 laboratory ©Inserm/Guénet, François
Highly-pathogenic agents: class 4 (or risk group 4) pathogens are highly pathogenic microorganisms characterised by a very high mortality rate, a lack of prophylactic or therapeutic measures to provide protection, and ready transmissibility. All class 4 pathogens currently known are viruses, and include viruses that cause haemorrhagic fevers or encephalitis. They include the Ebola, Marburg, Lassa, Junin, Machupo, Guanarito, Sabia, Crimean-Congo, Nipah and Hendra viruses.
The Jean-Mérieux P4 laboratory is the French partner of the European ‘EMP4’ project, coordinated by German researchers. As part of this project, a mobile P4 laboratory was deployed in Guinea to provide field assistance diagnosing Ebola cases. Six specialists in dangerous infectious diseases from the European Mobile Laboratory (EMLab) project arrived in Guéckédou last April and were relieved by seven new experts at the end of July. The mobile laboratory unit set up on site provides easily-transported equipment to enable the virus to be handled safely enclosed in boxes. This considerably improves the quantity of samples available for analysis and makes it easier to confirm cases of Ebola, so contributing to reducing the number of undiagnosed cases and preventing the spread of the disease.
In France, the French National Alliance for Life Sciences and Health (Aviesan), of which Inserm is a founder member, is mobilising its experts, at regular meetings, in order to define needs and consider directions for research to deal with future epidemics.
Are treatments for Ebola available?
Research on Ebola virus should put a priority on improving therapeutic treatments for the sick, whether by using treatments to limit replication of the virus or to boost protection of the host. This is a major need because, apart from symptomatic treatment (to relieve the pain but not treat its cause), there is currently no effective treatment and no molecule has been tested in an epidemic situation. The challenge is therefore to develop antivirals against Ebola.
There are several experimental vaccines and treatments against the virus that have given promising laboratory results. Several candidate vaccines have actually shown some efficacy when administered very soon after infection, but none when given more than two days after infection. A study published recently by German research teams used a mouse model to show that administering a derivative of pyrazinecarboxamide (T-705) orally 6 days after the beginning of the infection had a 100% effect on survival of the animals.
In France, research has particularly been conducted on other antiviral molecules as well as on the use of polyclonal antibodies.