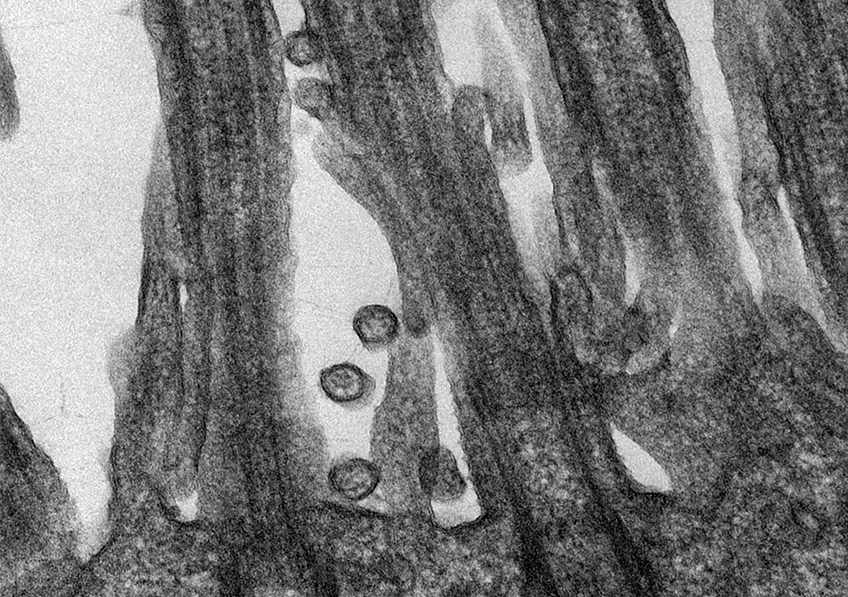
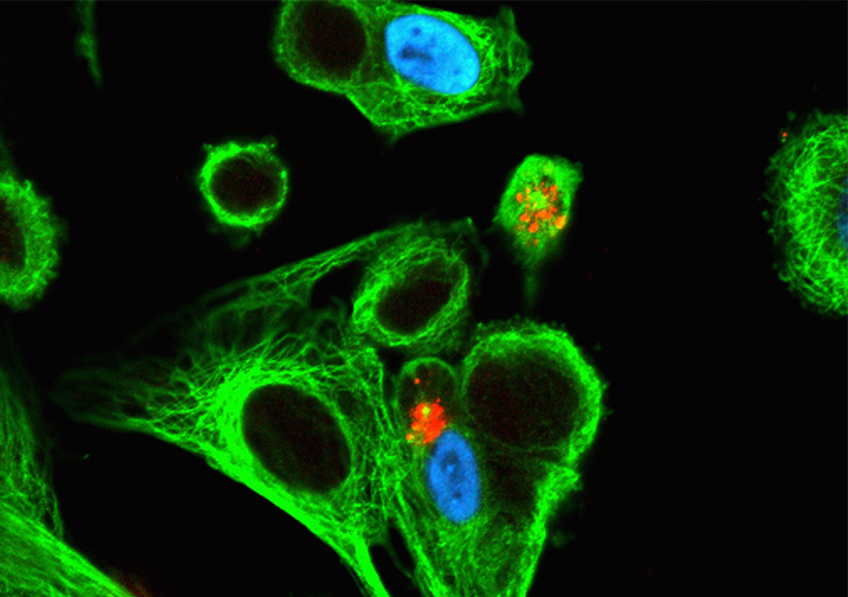
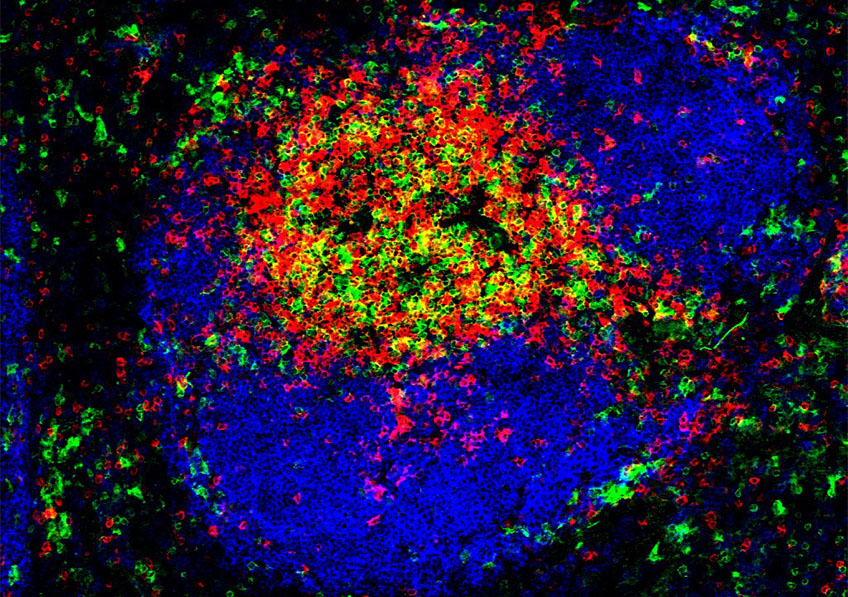
©MESRI/XR Pictures
At a time when the Sars-CoV-2 epidemic is continuing to spread, France’s Alliance for Life Sciences and Health (Aviesan) is mobilizing to accelerate research into the virus and COVID-19 disease through REACTing – a consortium coordinated by Inserm. With the support of the Ministry of Solidarity and Health and the Ministry of Higher Education, Research and Innovation, the Scientific Advisory Board of REACTing has selected 20 scientific initiatives covering diverse fields, from mathematical modelling to disease prevention and treatment.
Since the emergence of the first cases at the end of 2019, implementing high quality research to contain Sars-CoV-2 as quickly as possible and improve the treatment of those infected have been the objectives of the French scientific community, under the egis of Aviesan and the REACTing network.
Aviesan is comprised of nine essential academic stakeholders, its founding members: France’s Atomic Energy Commission (CEA), National Center for Scientific Research (CNRS), National Research Institute for Agriculture, Food and the Environment (INRAE), Institute for Research in Computer Science and Automation (INRIA), National Institute of Health and Medical Research (Inserm), Institut Pasteur, Research Institute for Development (IRD), Association of University Presidents (CPU), and Association of CEOs of Teaching and Regional Hospitals. The REACTing consortium is coordinated by Inserm.
Following a call for applications made to research teams across France, the Scientific Advisory Board of REACTing – a veritable research acceleration consortium – has selected 20 projects from a variety of scientific disciplines. Chosen for their effective and exhaustive contributions to knowledge production and to fighting this new epidemic, these projects have been categorized as follows:
- Diagnostic, clinical and therapeutic research projects
- Epidemiology research projects
- Fundamental research projects
- Human and social science research projects
Diagnostic, clinical and therapeutic research projects
In terms of therapeutic research, the projects selected concern the repurposing of existing medicines used in other diseases and the study of neutralizing monoclonal antibodies.
A clinical trial sponsored by Inserm will be set up in order to evaluate and compare four therapeutic combinations: remdesivir, lopinavir, the lopinavir+interferon combination, each combined with standard of care (non-specific and symptomatic treatments), and finally standard of care alone. A total of 3200 people will be enrolled, 800 of whom in France. This is an “adaptive” clinical trial in which ineffective compounds will be abandoned and any that appear to be useful will be tested.
Finally, one of the selected projects will analyze the accessibility of assisted ventilation protective masks and their integration in the healthcare offering.
Epidemiology research projects
Three of the selected projects concern epidemiology and modelling of the epidemic in order to better anticipate the spread of the virus by geographical area. One of the projects involves setting up an observational cohort sponsored by Inserm. Comprising all infected patients in France, this cohort will form the scientific basis for future studies.
Fundamental research projects
Three projects have been selected in the field of fundamental research, notably to further understanding of the in vitro viral replication context.
A research group will look at the animal reservoir issue, with a study evaluating the risks of virus transmission in the Mekong Delta region.
Human and social science research projects
The human and social sciences, which shed their own unique light on the epidemic and enable deeper understanding of the response of the public authorities and society as a whole, are also given pride of place. The leaders of these projects will look at the confinement of those repatriated from Wuhan, the online circulation of scientific data and their effects during the health crisis, and the modes of communication in the context of an emerging disease, in order to better guide public policy.
French research in Europe
French research is also swinging into action at the European level with the coordination of the Rapid European COVID-19 Emergency Response (RECOVER) project. Funded by the European Commission, it involves 10 international partners and its multiple components include epidemiological, clinical, and social science studies.
France is also participating in the research projects Fight-nCoV (Fighting-Off Coronavirus (Sars-Cov-2) With Broad-Spectrum Antivirals: Establishing Animal Viral Challenge Model), I-MOVE-COVID-19 (Multidisciplinary European network for research, prevention and control of the COVID-19 Pandemic) and CoNVat (Combating 2019-nCoV: Advanced Nanobiosensing platforms for POC global diagnostics and surveillance).
Through the deployment of these high quality, ambitious and relevant research projects, the REACTing community is doing everything it can to tackle the challenges of Sars-CoV-2 spread and the ensuing impacts on health and society.
The selected projects
THEME | SUMMARY | LEADER |
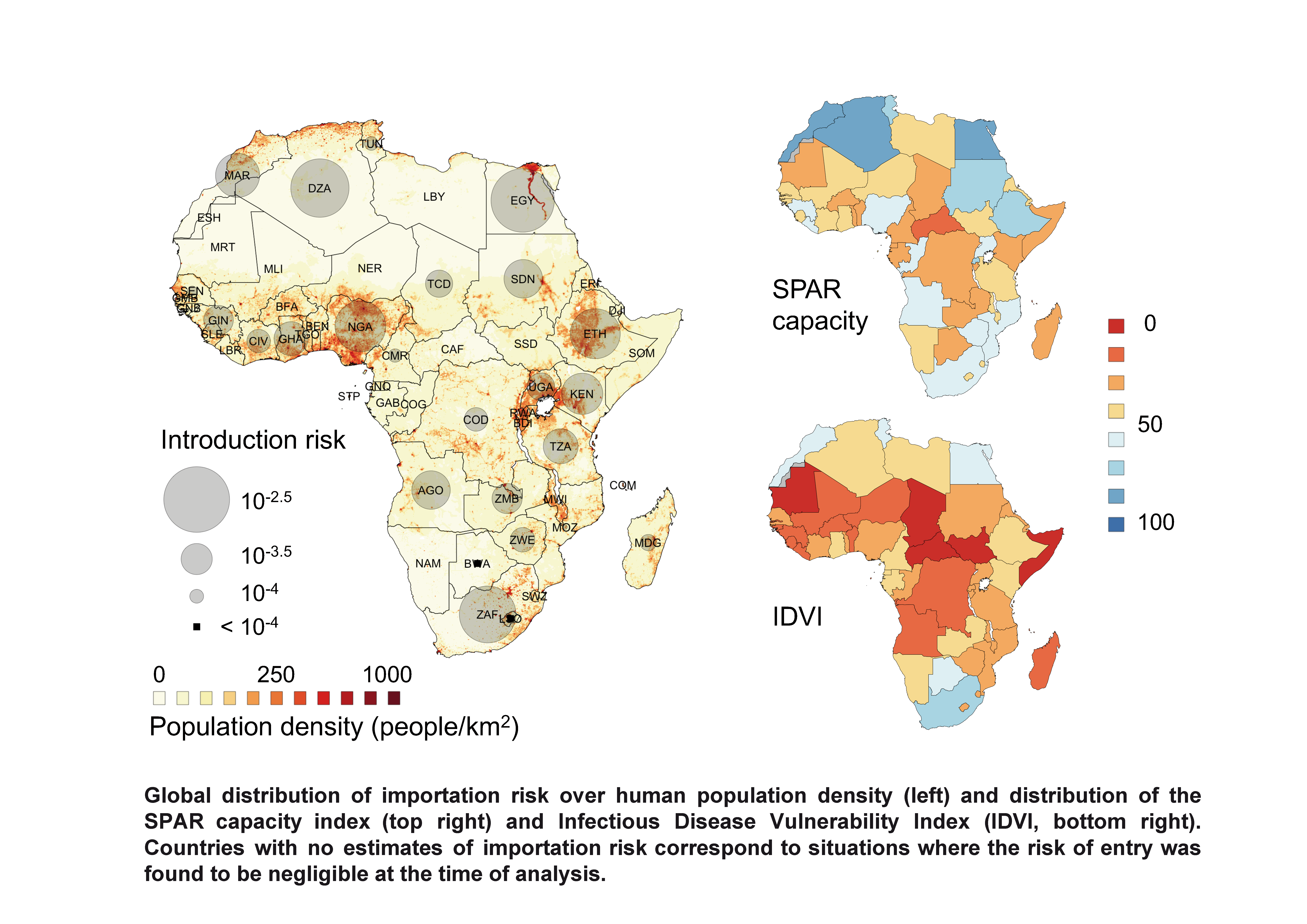
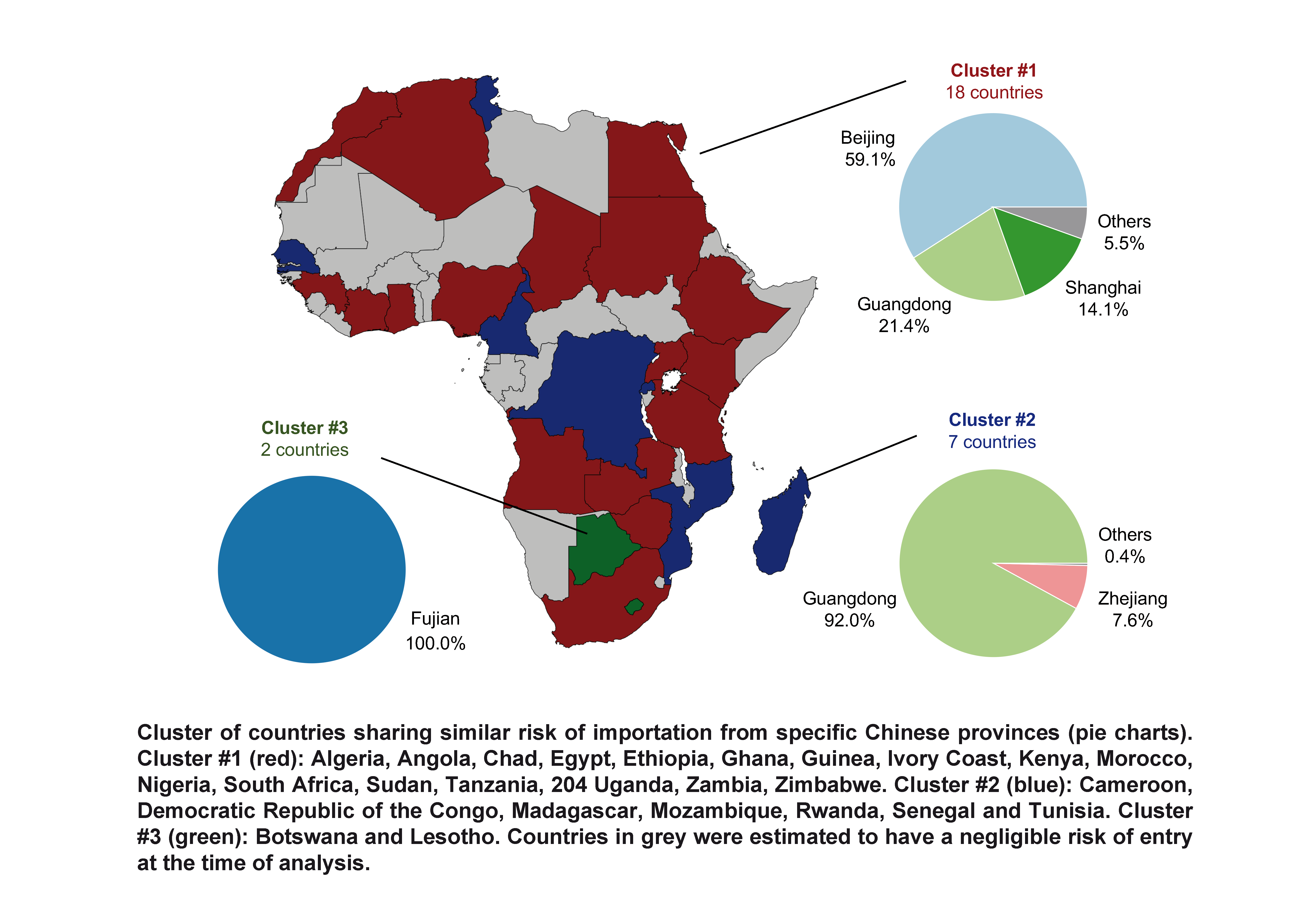
Epidemiology | Mathematical modelling to anticipate risk of 2019-nCoV importation by geographical area. | Vittoria Colizza
Inserm, Sorbonne Université Pierre Louis Institute of Epidemiology and Public Health |
Epidemiology | Monitoring of a cohort of all infected patients in France: a viral kinetics study in untreated patients and a pharmacokinetics and pharmacodynamics (PK/PD) study of those receiving experimental therapies (remdesivir). | France Mentré
Inserm, Université de Paris, Université Paris 13 Infection, Antimicrobials, Modelling, Evolution (IAME) unit |
Diagnostic, clinical and therapeutic research | Identification and characterization of human monoclonal antibodies neutralizing 2019-nCoV with the potential for development towards vaccine candidates. | Hugo Mouquet
Inserm, Institut Pasteur Humoral Immunity unit |
Human and social sciences | Use of the social sciences to inform public policy in terms of communication in the event of an emerging epidemic, based on social media treatment of the 2019-nCoV epidemic. | Laetitia Atlani-Duault
Inserm, IRD, Université de Paris Health, Gender and Vulnerability in Developing Countries unit |
Epidemiology | Monitoring of subjects with confirmed exposure to the novel 2019 coronavirus through virology and immunology studies. | Xavier Duval
Inserm, Université de Paris, Université Paris 13 Infection, Antimicrobials, Modelling, Evolution (IAME) unit
Bichat Clinical Investigation Center |
Fundamental research | Development of a replicon for coronavirus Covid-19. | Dr. Jean-François Eléouët INRAE Molecular Virology and Immunology unit |
Fundamental research | Potentiating existing nucleoside therapies. | Bruno Canardet Etienne Decroly CNRS, Aix-Marseille Université Architecture and Function of Biological Macromolecules laboratory |
Fundamental research | Implementation of an experimental model of SARS-CoV-2 infection in the cynomolgus monkey. | Roger Le Grand
Inserm, CEA, Université Paris-Saclay National Infrastructure for Biology and Health (IDMIT) |
Diagnostic, clinical and therapeutic research | Establishment of an antibody profile in convalescing patients and preparation of a serological test applied to an epidemiological survey in people exposed to SARS-Cov-2. | Marc Eloit
Institut Pasteur Pathogen Discovery laboratory |
Diagnostic, clinical and therapeutic research | Evolution of SARS-Cov-2 in the human host during infection and humoral response. | Sylvie van der Werf
Institut Pasteur, CNRS National Reference Center for Respiratory Viruses, Molecular Genetics of RNA Viruses |
Fundamental research | Live animal and endangered wildlife markets: a study evaluating the risks of COVID-19 transmission in the Mekong Delta region. | Philippe Dussart
Institut Pasteur in Cambodia |
Fundamental research | Role of furins in SARS-CoV-2 Spike protein maturation: evaluation of the antiviral potential of furin inhibitors | Bruno Coutard
Aix-Marseille Université, CNRS Emergence of Viral Pathologies laboratory, Polytech Marseille |
Diagnostic, clinical and therapeutic research | Strategy of repurposing medicines to treat 2019-nCoV infections | Bruno Lina
Inserm, Université Claude Bernard Lyon 1, École Normale Supérieure, CNRS International Center for Research on Infectious Diseases – CIRI |
Fundamental research | Proof of concept for the rapid production of recombinant SARS-CoV-2 | Julien Mélade
Inserm, IRD, Aix-Marseille Université, French Blood Establishment, École des Hautes Études en Santé Publique Emerging Viruses unit |
Human and social sciences | The aim of the AEC2-France project is to document and analyze, through anthropology research, the organized confinement for French nationals repatriated from Wuhan, epicenter of the Covid-19 epidemic | Marc Egrot IRD, Aix-Marseille Université Population-Environment-Development laboratory |
Human and social sciences | General population and healthcare professional knowledge, perceptions and behaviors in Metropolitan France in the face of the Covid-2019 epidemic | Thomas Hanslik
Inserm, Sorbonne Université Pierre Louis Institute of Epidemiology and Public Health |
Fundamental research | Multidisciplinary project combining artificial intelligence methods with proteins biochemistry. Aims to (1) reconstitute the COVID-19 replication complex in vitro; (2) model it in silico and (3) test nucleotide analog inhibitors (active on other viruses) and protein inhibitors (nanobodies) that will target the protein/protein interactions. | Isabelle Imbert
Aix-Marseille Université, CNRS Architecture and Function of Biological Macromolecules laboratory, Polytech Marseille |
Diagnostic, clinical and therapeutic research | Implantation of an assisted ventilation protective mask: acceptability and incorporation in the organization of care. | Jean-Christophe Lucet Inserm, Université de Paris, Université Paris 13 Infection, Antimicrobials, Modelling, Evolution (IAME) unit |
Human and social sciences | The aim of this project, which mobilizes data collected online and via interviews, is to produce an analytical description of the circulation of scientific data and their principal effects and a framework of analysis combining scientific and political challenges with a view to future research projects. | Guillaume Lachenal Science Po Médialab Daniel Benamouzig CNRS, Sciences Po Center for the Sociology of Organizations |
Diagnostic, clinical and therapeutic research | Randomized, multicenter, adaptive study of the efficacy and safety of treatments for hospitalized patients presenting with COVID 2019 infection | Florence Ader Inserm, CNRS, Université Claude Bernard Lyon 1, École Normale Supérieure de Lyon International Center for Research on Infectious Diseases (CIRI) |