Growth hormone deficiency is a common complication of radiotherapy. © Adobe Stock
Teams from Bicêtre AP-HP hospital, Inserm, Gustave Roussy and the University of Paris-Saclay studied the influence of growth hormone treatment on the risk of a second tumor. in 2,852 adults recovered from childhood cancer. The data confirm that treatment with growth hormone in these children with growth hormone deficiency does not increase the risk of developing a second cancer. This study therefore provides reassuring data on the long-term fate of these children cured of cancer and treated with growth hormone to enable them to reach normal adult height. The results of this study were published in the European Journal of Endocrinology in September 2020.
Growth hormone deficiency is a common complication of brain radiation therapy. Children treated with radiation therapy need growth hormone treatment to reach normal adult height, but there have been concerns about a possible increased risk of another tumor developing in adulthood caused by it. growth hormone treatment.
Researchers from unit 1018 of the “Center for Research in Epidemiology and Population Health (CESP)” (Inserm / Université Paris-Saclay / Gustave Roussy) and from Bicêtre AP-HP hospital, analyzed data from a French cohort, Euro2k, which brings together 2,852 survivors of pediatric cancer diagnosed before the age of 18 before 1986. Among them, 196 had been treated in childhood with growth hormone.
The research team studied the influence of growth hormone treatment on the occurrence of second tumors with a follow-up of 26 years, taking into account the doses of radiation received by all the organs of the body. These were obtained by reconstituting the radiotherapy received for each child.
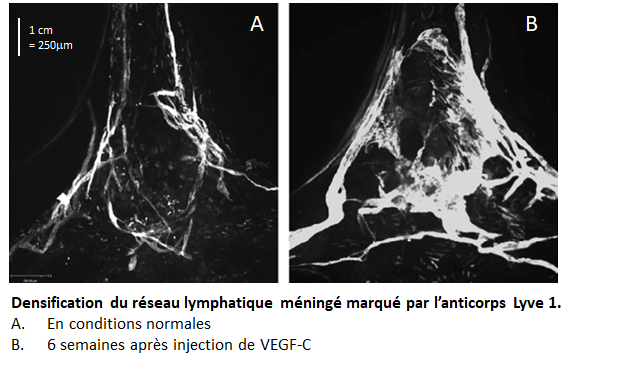
In this cohort, 374 survivors developed a second tumor, 40 of whom received growth hormone treatment in childhood. Analysis of the data shows that treatment with growth hormone is not associated with an increased risk of second tumors. However, these researchers found in survivors who received growth hormone treatment for more than 4 years, a slight increase (x2) risk of meningioma, a benign tumor of the meninges favored by high doses of radiotherapy. This slight excess risk of meningioma in survivors who received more than 4 years of treatment with growth hormone is not significant, however, and there is no evidence that the treatment with growth hormone either. responsible.
“This study provides information on the long-term fate of the children whom we treat with growth hormone for a growth hormone deficiency secondary to the treatment of their cancer. These new data allow us to approach the treatment with growth hormone calmly. in these children cured of cancer, when necessary and to reassure families about the absence of an increased risk of second tumors during this treatment. “ concludes Dr Cécile Thomas-Teinturier, pediatrician-endocrinologist at the Bicêtre AP-HP hospital and first author of the study.