The HOMAGE (Heart OMics in AGEing) project, coordinated by the French National Institute of Health and Medical Research (INSERM), has been awarded a grant by the European Commission for a 6 year period. The project aims to identify and validate specific biomarkers of heart failure in order to prevent the development of the disease affecting elderly population. 17 research groups from 10 countries will collaborate to investigate new ways of preventing heart failure. The project will use an innovative ‘omic-based’ approach which investigating simultaneously a huge amount of genes, proteins and metabolites.
The 17 partners will meet at Nancy on February 22nd for the kick off meeting of HOMAGE.
Professor Faiez Zannad, Head of the Centre d’Investigation Clinique Pierre Drouin Inserm U9501 and Inserm Unit 1116 based in Nancy, is the project coordinator. The 12 million euros grant of the European Commission will be dedicated to the HOMAGE consortium for research on heart failure, a serious illness altering myocardial activity which affects more than 6.5 million persons in Europe. Indeed, the prevalence of heart failure is increasing worldwide due to an ageing population as well as a rising trend of risk factors for heart disease such as diabetes, obesity and hypertension.
Heart failure is a major cause of mortality and morbidity in the world and remains the most frequent cause of hospitalization for patients over 65 years old.
The costs related to heart failure have been estimated around 1.5 billion euros per year in France[1].
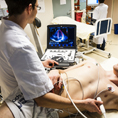
Photo : ©Serimedis/Inserm
Despite important progress in the treatment including new drugs, new medical devices and innovative disease management programmes, the diagnosis of heart failure is often difficult in older adults with co-morbidities. Screening tests are usually based on blood pressure, glycaemic and cholesterol control. Although they are useful to detect high risk patients, they are limited regarding their sensitivity and specificity. During the past decade, promising biomarkers such as natriuretic peptides have been identified to diagnose heart failure, but their predictive value remains relatively poor. The HOMAGE consortium is willing to validate more specific and more sensitive biomarkers which should facilitate an early detection of the disease in patients at risk.
To achieve this goal, the consortium agreed on the use of an ‘omic-based’ approach. This approach aims to validate promising biomarker candidates by crossing a large volume of data (genomics, proteomics, miRNomics, transcriptomics and metabolomics). This would permit scientists to understand new pathophysiological mechanisms, signaling pathways and identify new therapeutic targets to prevent heart failure.
The HOMAGE consortium will manage cohorts for a total of 30 000 patients. The European researchers will firstly identify biomarker candidates in blood and study their predictive value for heart failure and common co-morbidities associated with ageing (renal impairment, cognitive disorders…). Subsequently, HOMAGE will lead a clinical trial to look for novel treatments of heart failure that can be targeted specifically to those patients at risk.
This trial will allow identifying patients’ omics based biomarker profiles most likely to predict response to treatment with the better benefit/risk ratio, an attempt into personalized medicine.
[1] Fédération Française de Cardiologie
The 17 partners of HOMAGE project : www.homage-hf.eu (en ligne le 21 février)
Inserm, France : https://www.inserm.fr/
Inserm U942/ Biomarqueurs et maladies cardiaques, France
Inserm UMR 1048/ Equipe 7, France
Inserm U744/ Recherche des Déterminants Moléculaires des Maladies Cardiovasculaires, France
Inserm Transfert, France : https://www.inserm-transfert.fr/
European Drug Development Hub, France : https://www.fondationtransplantation.org
ACS Biomarker, Pays-Bas : https://acsbiomarker.com/
Randox Testing Service, Royaume-Uni : https://www.randoxtestingservices.com/
Medical University of Graz, Autriche : https://www.meduni-graz.at/en/
University of Manchester, Royaume-Uni : www.manchester.ac.uk
Fundación para la Investigación Médica Aplicada, Espagne : www.cima.es
University College Dublin, Irlande : www.ucd.ie
University of Hull, Royaume-Uni : www.hull.ac.uk
Maastricht University, Pays-Bas : https://www.maastrichtuniversity.nl/
Istituto di Ricerche Farmacologiche ‘Mario Negri’, Italie : https://www.marionegri.it/mn/en/
Hannover Medical School, Allemagne : https://www.mh-hannover.de
University of Leuven, Belgique : www.kuleuven.be/english/
London School of Hygiene, Royaume-Uni : https://www.lshtm.ac.uk/
Emory University, Etats Unis : https://www.emory.edu
University of Glasgow, Royaume-Uni : https://www.gla.ac.uk/
Collaborative institutions:
The Trustees of Boston University, National Heart, Lung, and Blood Institute’s Framingham Heart Study, Etats Unis
Imperial College, Royaume-Uni
Steno Diabetes Center (Novo Nordisk), Danemark