A study financed by the Assistance Publique-Hôpitaux de Paris[1] has been conducted under the direction of Monica Zilbovicius[2] in the Inserm Unit 1000 on a particular region of the brain, the superior temporal sulcus (STS), influencing perception and behaviour of the gaze. This work has shown that transcranial magnetic stimulation (non-invasive and painless) of the STS can selectively and transiently inhibit the subject’s gaze into the eyes of the person speaking to them. Published in the journal Cerebral Cortex, it offers new therapeutic prospects for autistic patients precisely presenting anatomical and functional differences of the superior temporal sulcus.
(c) Monica Zilbovicius / Inserm
It is commonly admitted that the gaze plays an essential role in social interactions. At a very young age, human beings look others in the eye, because information from the eyes allows us to guess their intentions and feelings. In the brain, many studies highlight the importance of a specific region of the brain, the superior temporal sulcus (STS), in perception and behaviour of the gaze. However, to date, no experimental data has demonstrated a possible modification of the gaze by artificial modulation of a neural network.
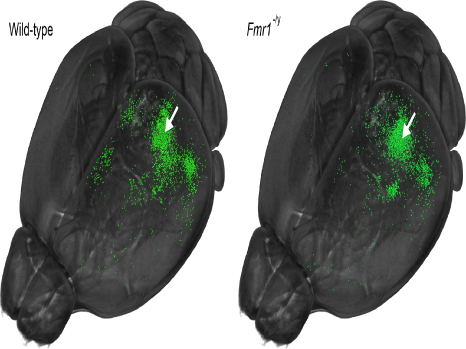
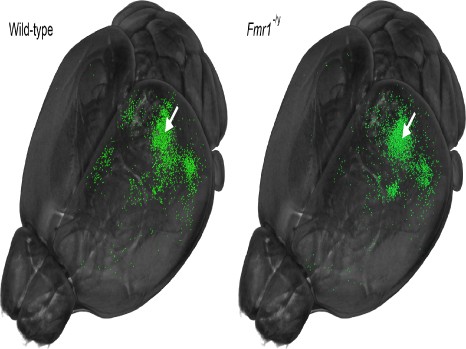
Work conducted by Inserm Unit 1000, financed by AP-HP, has confirmed that ad hoc intervention in the STS was able to have an impact on the behaviour of the gaze. The researchers used transcranial magnetic stimulation (TMS): this method consists of applying a non-invasive and painless magnetic impulse to the brain through the skull, in order to study changes of gaze caused by inhibition of the STS by TMS, using oculometry (‘eye-tracking’). They showed 15 subjects films of actors and recorded the way they looked at these films before and after inhibition of the STS. In this way the researchers observed a significant distancing from the gaze of control subjects relative to the eyes of the actors, compared to the base measurement (cf. pictures). Inhibition of the superior temporal sulcus therefore selectively and transiently disrupts the movement of the subject’s gaze into the eyes of another subject.
These results offer new therapeutic prospects for autistic patients. In fact, many brain imaging studies have revealed the presence of anatomical and functional differences of the STS in this type of patient not displaying a marked preference of other people’s eyes.
For Prof Monica Zilbovicius, “given that TMS can be applied so as to inhibit or stimulate a certain brain area, stimulating the STS using TMS could cause an increase in gazing into the eyes. This is an avenue we will explore during the next stage of our research”.
[1] French Hospital clinical research programme (PHRC)
[2] Inserm Unit 1000, Paediatric Radiology Department, Necker Hospital for Sick Children, AP-HP