Yehezkel Ben-Ari, Founder and Honorary Director of INMED (Institut de Neurobiologie de la Méditerranée), INSERM, and Eric Lemonnier, a clinician specialising in autism at the CHRU of Brest, recently published the results of a double-blind clinical trial to evaluate the usefulness of a diuretic in the treatment of autism. Sixty children between 3 and 11 years old with autism or Asperger’s syndrome were treated for 3 months either with a diuretic to reduce their intracellular chloride levels or with a placebo. Although this therapy is not curative, it nevertheless reduced the autistic disorders’ severity in three-quarters of the children. The researchers have filed a request for authorisation to perform a multi-centre European clinical trial in order to determine more precisely the population concerned by this therapy.
Details of this work have been published in the Translational Psychiatry review dated 11 December 2012.
Contribution made by the fundamental research on neuronal chloride
Previous work carried out by the team of researchers led by Yehezkel Ben-Ari in INSERM unit 901, the Institut de Neurobiologie de la Méditerranée (INMED) in Marseille, on intracellular chloride concentrations have demonstrated that they are abnormally high in immature neurons or neurons previously affected by epileptic seizures or other cerebral lesions. Many anxiolytics, analgesics and antiepileptics act by increasing the effects of GABA – the brain’s main chemical mediator – which normally inhibits the neurons. When the cells contain a very high chloride concentration, however, GABA’s effects are reversed. GABA no longer inhibits the neurons; the anxiolytic molecules accentuate these effects instead. These molecules have an excitatory effect, aggravating the disorder rather than alleviating it[1]. This is what has been observed in the case of epilepsy: diazepam, an anxiolytic, actually aggravated the seizures in certain situations. The research team then showed the benefits of a diuretic in mitigating this effect.
From fundamental research to clinical research
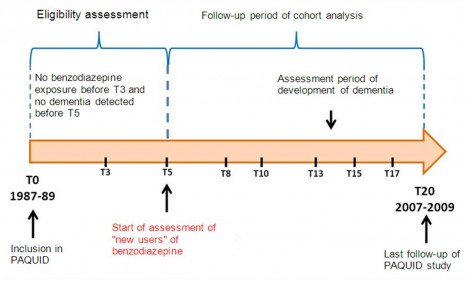
Indirect experimental data suggest that the inhibitory transmitter GABA’s action is modified in autism. Eric Lemonnier, a clinician at the CHRU of Brest, pointed out to Yehezkel Ben-Ari that valium is not prescribed to children suffering from autism because their parents say they become more agitated as a result, suggesting that, as in epilepsy and other brain pathologies, their intracellular chloride concentration is increased. This encounter led to the idea of testing a diuretic – in the same way as for epilepsy – to determine whether this could alleviate autistic disorders. A pilot study in 5 children was rapidly set up in 2010 because bumetanide, the diuretic tested, is in common use, particularly in treating high blood pressure. The taking of these molecules can, however, lower the potassium level, meaning that a potassium supplement is required. The researchers then began a randomised double-blind clinical trial in 60 children between 3 and 11 years old with autism or Asperger’s syndrome.
Reduction in the severity of autistic disorders
The children were monitored for 4 months. One group was treated with the diuretic (1 mg of bumetanide) while a placebo was administered to the second group for 3 months. No treatment was administered in the final month. The severity of the children’s autistic disorders was rated at the beginning of the test, the end of the treatment, i.e. after 90 days and one month after the test ended.
After 90 days of treatment, the mean CARS (Childhood Autism Rating Scale) test score of the children treated with bumetanide had significantly improved. The severity of the treated group’s autistic disorders shifted from high (> 36.5) to medium (< 36.5). No significant difference was observed in the score of the group treated with the placebo, however. In total, the clinical diagnosis of 77% of the children who received the treatment improved in the Clinical Global Impressions (CGI) test. When the treatment was terminated, some disorders reappeared. The treatment with bumetanide is therefore reversible.
The widely-applied Childhood Autism Rating Scale (CARS) behavioural scale was used to rate the severity of the disorders, based on videos of the children’s behaviour during an activity led by a caregiver. The films were analysed with the assistance of their parents. A rating is obtained from the analysis as follows: if the rating is between 30 and 36, the child suffers from a moderate or average disorder; if the rating is higher than 36, the child is severely autistic.
Two other indicators were used to assess the severity of the disorders: the Clinical Global Impressions (CGI) clinical diagnosis, and the Autism Diagnostic Observation Schedule – Generic (ADOS–G) indicator combining assessment criteria such as social interaction and communication.
Dr. Lemonnier explained the case of a 6-year-old boy:
“Prior to the treatment, the child presented with low language abilities and little social interaction, was hyperactive and exhibited constantly-combative behaviour. After three months of treatment, his parents, teachers, the hospital nursing staff and his friends at school all said that he was participated more, particularly in the games proposed by the psychologist. His attention and eye contact also improved.”
“Even though it is not curative, the diuretic reduced the severity of most of the children’s autistic disorders. According to the children’s parents, they are more “present””
, added Yehezkel Ben-Ari.
Given the population’s heterogeneity, the researchers assume that the treatment could act differently depending on the severity of the autistic disorders. By forming groups based on severity, the results suggest that the treatment would be more effective in the least seriously-affected children.
As a result, the researchers have filed an authorisation request for a multi-centre European clinical trial in order to determine more precisely the population concerned by this treatment and ultimately obtain a marketing authorisation for this therapy. This test is supervised by a company created by Prof. Ben-Ari and Dr. Lemonnier (Neurochlore). Analyses are also essential in order to assess the long-term effects of taking these molecules and the required dose. Lastly, the researchers stress the need to continue the work on experimental models to determine how chloride is regulated and how it is deregulated in the neural networks of autistic patients.
A patent application has been filed for this work, and a licence has been granted to the Neurochlore start-up. Neurochlore has received funding from the French National Research Agency (ANR) (in the Biomedical Innovation in public-private Research Partnership (BIRP) “Cure Autism” project).
[1] See diagram on p. 3 “Further details”